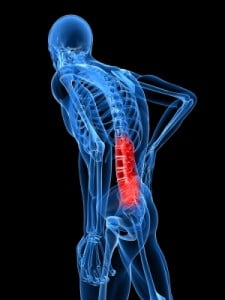
There’s nothing better than snuggling into a good book. But are you experiencing back pain while sitting and reading for an extended period? Back pain can often be caused by improper posture. While reading, whether using a physical book or an electronic device, many people experience back pain in the neck and shoulder or in the low back. Here are some ways to alleviate back pain while reading.
Reading can cause strain on the neck and shoulders if there is a tilt in the neck to look down at your book or device. While sitting and reading, it’s important to place your reading material at eye level. Sitting with your head leaning forward and back hunched can cause hyperflexion of the cervical spine and lead to severe neck and back pain over time. It is best to use a stand that can be adjusted to the required height. Many have recommended raising your materials with your hand; however, this may also cause some strain on the neck and shoulders. While holding an object in front of you at eye level, either with one or both hands, your shoulder and neck muscles are in constant contraction to sustain this positioning. Even over a period of a few minutes, this can cause the muscles to spasm or cause intense strain. Using an adjustable stand will ensure that we can sit straight up, taking pressure off of the cervical spine.
The best posture for reading is sitting upright in a chair with lumbar support. Avoid sitting on a seat that lacks back support such as a stool or a bench. A chair with good ergonomics is one that supports the low back and provides an arm rest to place both elbows. Mentioned above, we want to avoid stiffness in the upper back and neck muscles. Placing your elbows on an arm rest that is low enough to support your arms without adding additional strain is ideal. A study examining the association of low back pain with cell phone use found that thoracolumbar kyphosis and lumbar lordosis (curvature in the spine causing a pelvis tilt) increased with prolonged sitting. Participants had a slouch and progressed spine curvature after sitting for longer than 30 mins. The study also found that those with pre-existing back pain had a significantly higher increase in lordosis and complained of more back pain. When sitting for longer than 30 minutes, take breaks. Sitting should be interrupted by standing breaks to keep blood flowing and reduce stiffness in muscles.
To summarize, here are some things we can do to minimize back pain while reading or using a device while sitting.
– Sit with back and arm support for your neck and shoulders
– Bring your reading material or device to eye level to avoid neck strain
– Take breaks and stand for a minute or so while sitting for more than 30 minutes
References
In TS, Jung JH, Jung KS, Cho HY. Spinal and Pelvic Alignment of Sitting Posture Associated with Smartphone Use in Adolescents with Low Back Pain. Int J Environ Res Public Health. 2021 Aug 7;18(16):8369. doi: 10.3390/ijerph18168369. PMID: 34444119; PMCID: PMC8391723.


 Some opioids, such as oxycodone, are often combined with Tylenol (
Some opioids, such as oxycodone, are often combined with Tylenol (
 Where to begin? In the first two chapters of my book, End
Where to begin? In the first two chapters of my book, End 
